This web page was produced as an assignment for Genetics 564, an undergraduate capstone course at UW-Madison.
What is APECED?
Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy (APECED), also known as autoimmune polyglandular syndrome 1 (ASP1), is a rare autosomal recessive disease caused by loss of function mutations in the Autoimmune Regulator (AIRE) gene [1]. Because AIRE is an autoimmune regulator, APECED is characterized by immune cell dysfunction, leading to multiple autoimmunities. APECED patients can have a wide range of symptoms which vary person to person. However, certain populations with high rates of APECED tend to have similar symptoms, suggesting some symptematic variation is due to the specific AIRE mutation [2]. These can include chronic mucocutaneous candidiasis (CMC), hypoparathyroidism, chronic adrenocortical insufficiency (Addison’s disease), and ectodermal dystrophy. APECED is more prevalent in some populations including Iranian Jews (1 in 9000), Finns (1 in 25,000) and Sardinians (1 in 14,000) [3]. Because it is so rare, the prevalence of APECED is challenging to determine. In the United States, APECED is estimated to affect 1 in every 2 to 3 million newborns [4]. Another study estimates that APECED affects almost 1 of every 100,000 people worldwide [5].
Unlike other systemic autoimmune diseases, APECED can be described by Mendelian inheritance because it is monogenic, meaning it is caused by a mutation in a single gene. As a monogenic recessive disease, APECED can be traced through familial lines and more easily studied because the cause, a mutation in AIRE, is known. The National Institute of Allergy and Infectious Diseases recognizes how important APECED is, and has said that studying APECED is a priority to better understand AIRE deficiency and uncover therapeutic targets [6].
Unlike other systemic autoimmune diseases, APECED can be described by Mendelian inheritance because it is monogenic, meaning it is caused by a mutation in a single gene. As a monogenic recessive disease, APECED can be traced through familial lines and more easily studied because the cause, a mutation in AIRE, is known. The National Institute of Allergy and Infectious Diseases recognizes how important APECED is, and has said that studying APECED is a priority to better understand AIRE deficiency and uncover therapeutic targets [6].
The AIRE gene
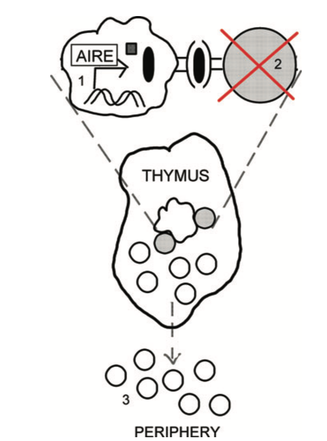 If a naive T-cell binds to an AIRE expressing mTEC in the thymus, it is eliminated because it is bound self-antigen that the mTEC was expressing. This process helps ensure self-reactive, autoimmune causing T-cells do not escape into the body.
If a naive T-cell binds to an AIRE expressing mTEC in the thymus, it is eliminated because it is bound self-antigen that the mTEC was expressing. This process helps ensure self-reactive, autoimmune causing T-cells do not escape into the body.
AIRE is a transcription factor that has many important roles in self-tolerance. When your body makes B and T cells (immune cells), the receptors are randomly generated meaning the antigen (a protein) they recognize is random. As a result, some newly generated immune cells have receptors that recognized self-antigen and, if let loose into the body, could be self reactive leading to autoimmune diseases.
The process of selecting against self-reactive T cells is called negative selection and occurs in the thymus, a primary lymphoid organ located between the heart and sternum. AIRE is highly expressed by medullary thymic epithelial cells (mTECs) which causes them to express tissue specific antigens that are normally found elsewhere in the body [7]. If T cells bind too tightly to tissue specific (self) antigens, they receive apoptotic signals which cause these self-reactive T cells to die (a process called clonal deletion) [8]. AIRE is essential in expressing these tissue specific antigens for negative selection.
In addition the role AIRE plays in the thymus, AIRE expression has been documented in other parts of the body including monocyte and dendritic cells (antigen presenting cells that activate T cells) found in secondary lymphoid organs and lymphoid stroma [9]. However, the function of AIRE in these cells is not fully understood.
The process of selecting against self-reactive T cells is called negative selection and occurs in the thymus, a primary lymphoid organ located between the heart and sternum. AIRE is highly expressed by medullary thymic epithelial cells (mTECs) which causes them to express tissue specific antigens that are normally found elsewhere in the body [7]. If T cells bind too tightly to tissue specific (self) antigens, they receive apoptotic signals which cause these self-reactive T cells to die (a process called clonal deletion) [8]. AIRE is essential in expressing these tissue specific antigens for negative selection.
In addition the role AIRE plays in the thymus, AIRE expression has been documented in other parts of the body including monocyte and dendritic cells (antigen presenting cells that activate T cells) found in secondary lymphoid organs and lymphoid stroma [9]. However, the function of AIRE in these cells is not fully understood.
How does AIRE loss of function leads to APECED?
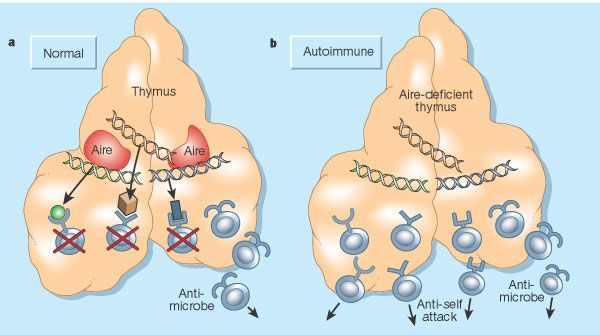
Loss of productive negative selection in the thymus is the main reason AIRE loss of function mutations is thought to cause APECED. Without AIRE, the mTECs do not express tissue specific antigens and therefore cannot test whether T cells are self-reactive. These self-reactive T cells in an AIRE deficient thymus are not killed, and are instead released into the body where they can cause a range of autoimmune diseases. However, studies have noted other changes in immune cells and/or signaling that are also thought to contribute to APECED symptoms. Overall, there are clear links between AIRE loss of function mutations and APECED [10], but details about the many effects of the AIRE mutation (beyond negative selection in the thymus) are not fully understood.
Autoantibodies, especially against cytokines which act as signaling molecules for the immune system, are another important phenotypic change found in APECED patients, For example, APECED patients have a high level of antibodies against type 1 interferons (IFN), signaling molecules that normally help activate immune responses to pathogens and stimulate adaptive immunity [11]. The overall phenotypic effect of these anti-IFN antibodies is still being investigated. Similarly, it has been observed that APECED patients have a defect in T-regulatory cell (Treg) activation, meaning APECED patients cannot suppress auto-reactivity and therefore lose immunological tolerance [12]. Furthermore, a longitudinal study found a correlation between the level of antibodies against IL-17A, a pro-inflammatory cytokine, and susceptibility to Chronic Mucocutaneous Candidiasis in APECED patients [13]. More research is needed to determine how these high levels of autoantibodies relate to APECED component diseases and how they are related to AIRE loss of function.
Autoantibodies, especially against cytokines which act as signaling molecules for the immune system, are another important phenotypic change found in APECED patients, For example, APECED patients have a high level of antibodies against type 1 interferons (IFN), signaling molecules that normally help activate immune responses to pathogens and stimulate adaptive immunity [11]. The overall phenotypic effect of these anti-IFN antibodies is still being investigated. Similarly, it has been observed that APECED patients have a defect in T-regulatory cell (Treg) activation, meaning APECED patients cannot suppress auto-reactivity and therefore lose immunological tolerance [12]. Furthermore, a longitudinal study found a correlation between the level of antibodies against IL-17A, a pro-inflammatory cytokine, and susceptibility to Chronic Mucocutaneous Candidiasis in APECED patients [13]. More research is needed to determine how these high levels of autoantibodies relate to APECED component diseases and how they are related to AIRE loss of function.
Symptoms associated with APECED
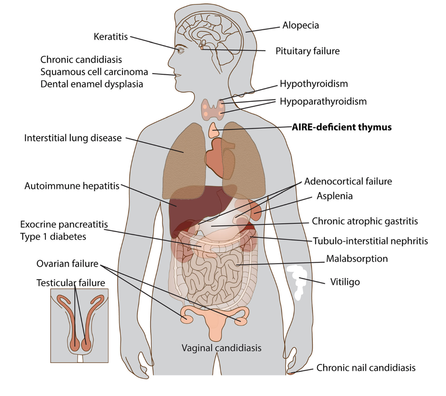
There are many signs and symptoms of APECED that can present at different ages. Not all patients have every component of APECED, but to be clinically diagnosed, patients must present with two of the following three conditions [14]:
- Chronic mucocutaneous candidiasis (CMC)
- Hypoparathyroidism,
- Adrenocortical insufficiency (Addison's disease)
1) Chronic mucocutaneous candidiasis (CMC) is a disorder characterized by persistent and reoccurring infections with Candida albicans, a yeast that normally lives on the skin and mucosa [17]. People with APECED get infections on their skin, nails, and mucosa, possibly due to an autoimmune response against IL-17F and IL-22 producing cells, which have anti-fungal functions [18].
2) Hypoparathyroidism is an endocrine disorder where parathyroid hormone (PTH) is produced at abnormally low levels by the parathyroid gland. Parathyroid hormone usually regulates calcium and phosphorous levels in the blood along with bone growth [19]. Low levels of PTH can cause many symptoms, including muscle cramps or spasms, twitching in around mouth and fingers, fatigue or weakness, headaches, patchy hair loss, and brittle nails [20]. Another sign of hypoparathyroidism is low levels of calcium and high levels of phosphorous in the blood [21].
3) Adrenocortical insufficiency (Addison’s disease) is another endocrine disorder where the adrenal glands do not produce a sufficient amount of cortisol and often aldosterone [22]. Cortisol is important for regulating blood pressure, metabolism, and inflammatory responses while aldosterone helps maintain blood pressure along with the sodium and potassium levels in the blood [23]. Common symptoms of adrenocortical insufficiency include chronic fatigue, muscle weakness, loss of appetite, abdominal pain and weight loss [24].
There are many other conditions associated with APECED that vary among individuals. The list below includes other conditions found among APECED patients, a description of the condition, and the prevalence of these conditions among APECED patients reported by clinical studies.
2) Hypoparathyroidism is an endocrine disorder where parathyroid hormone (PTH) is produced at abnormally low levels by the parathyroid gland. Parathyroid hormone usually regulates calcium and phosphorous levels in the blood along with bone growth [19]. Low levels of PTH can cause many symptoms, including muscle cramps or spasms, twitching in around mouth and fingers, fatigue or weakness, headaches, patchy hair loss, and brittle nails [20]. Another sign of hypoparathyroidism is low levels of calcium and high levels of phosphorous in the blood [21].
3) Adrenocortical insufficiency (Addison’s disease) is another endocrine disorder where the adrenal glands do not produce a sufficient amount of cortisol and often aldosterone [22]. Cortisol is important for regulating blood pressure, metabolism, and inflammatory responses while aldosterone helps maintain blood pressure along with the sodium and potassium levels in the blood [23]. Common symptoms of adrenocortical insufficiency include chronic fatigue, muscle weakness, loss of appetite, abdominal pain and weight loss [24].
There are many other conditions associated with APECED that vary among individuals. The list below includes other conditions found among APECED patients, a description of the condition, and the prevalence of these conditions among APECED patients reported by clinical studies.
- Intestinal dysfunction in APECED patients can take many forms including diarrhea, constipation, or malabsorption of nutrients. Intestinal dysfunction and the accompanying symptoms can be caused by intestinal candidiasis, hypocalcemia resulting from hypoparathyroidism, failure of the pancreas to secrete enzymes necessary for digestion, autoimmune endocrinopathy (where enteroendocrine cells in the GI tract are targeted), or other autoimmunities [25]. Intestinal dysfunction was reported in about 25% of APECED patients [26].
- Ectodermal manifestations come in many forms including vitiligo (blotchy loss of skin color), nail dystrophy (damage), alopecia areata (patchy hair loss), candida infections of the nails and surrounding tissue (in 72% of patients) [27], or keratoconjunctivitis (inflammation of the cornea and conjunctiva) [28] Other, less common, dermatological manifestations can include scleroderma (hardening of the skin), Sjogren’s syndrome (dry eyes and mouth), lichen planus (skin inflammation leading to purplish bumps), and oral squamous cell carcinomas [29].
- Type 1 Diabetes occurs as a result of pancreatic autoimmunity. APECED patients with type 1 diabetes have high titers of self-reactive antibodies (such as anti-glutamic acid decarboxylase or anti-insulin). The prevalence of type 1 diabetes ranges from 1 to 18% in previous studies of APECED patients, with a higher prevalence in Finnish APECED populations [30].
- Gonadal insufficiency occurs in both males and females with APECED. In females, ovarian insufficiency often occurs in the teenage or early adult years and in about two thirds of females with APECED. Ovarian insufficiency is correlated with autoantibodies against side-chain cleavage enzymes. The biochemical signs of ovarian failure are high follicle stimulating hormone (FSH) and luteinizing hormone (LH) along with low oestrogen. Starting oestrogen replacement at pubertal age can be used to maintain normal female development which is usually arrested, especially in people with the aforementioned biochemical signs [31]. In males, testicular insufficiency can occur during adulthood but with lower prevalence: 25% in Finnish patients and lower in overall APECED populations. The lower rate of testicular insufficiency compared to ovarian insufficiency can be explained by the blood-testis barrier which prevents interactions between the testes and immune cells [32].
References
[1] Finnish-German APECED Consortium. 1997. An autoimmune disease, APECED, caused by mutations in a novel gene featuring two PHD-type zinc-finger domains. Nature. https://www.ncbi.nlm.nih.gov/pubmed/9398840/
[2] Peterson et al. 2003. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy (APECED): a model disease to study molecular aspects of endocrine autoimmunity. Clinical Experimental Immunology.
[3] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome. Annals of the New York Academy of Science. http://onlinelibrary.wiley.com/doi/10.1111/j.1749-6632.2011.06308.x/epdf
[4] National Organization for Rare Disorders. Autoimmune Polyglandular Syndrome Type 1. https://rarediseases.org/rare-diseases/autoimmune-polyglandular-syndrome-type-1/
[5] Hayter and Cook. 2012. Updated assessment of the prevalence, spectrum and case definition of autoimmune disease. Autoimmunity Reviews. Vol 11. http://www.sciencedirect.com/science/article/pii/S1568997212000225
[6] National Institute of Allergy and Infectious Diseases. Autoimmune Polyglandular Syndrome Type 1 (APS-1). https://www.niaid.nih.gov/diseases-conditions/autoimmune-polyglandular-syndrome-type-1-aps-1
[7] Gardner et al. 2009. AIRE in the thymus and beyond. Current opinion in immunology. 21:582–589.
[8] Owen, Punt, Stranford, and Jones. 2013. Kuby Immunology 7th edition. p. 310
[9] Gardner et al. 2009. AIRE in the thymus and beyond. Current opinions in immunology.
[10] The Finnish-German APECED Consortium. 1997. An autoimmune disease, APECED, caused by mutations in a novel gene featuring two PDH-type zinc-finger domains. Nature genetics volume.
[11] Kisdand et al. 2010. Chronic mucocutaneous candidiasis in APECED or thymoma patients correlates with autoimmunity to Th17-associated cytokines. The Journal of Experimental Medicine.
[12] Laasko et al. 2010. Regulatory T cell defect in APECED patients is associated with loss of naive FOXP3+ precursors and impaired activated population. Journal of Autoimmunity.
[13] Sarkadi et al. 2014. Autoantibodies to IL-17A may be correlated with the severity of mucocutaneous candidiasis in APECED patients. Journal of Clinical Immunology.
[14]Seattle Children's Hospital. Autoimmune Polyendocrinopathy, Candidiasis, Ectodermal Dystrophy (APECED).http://www.seattlechildrens.org/healthcare-professionals/access-services/diagnostic-services/laboratories/immunology-diagnostic-laboratory/disorders/apeced/
[15] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[16] Betterle and Volpato. 1998. Adrenal and ovarian autoimmunity. European Journal of Endocrinology. Vol 138. http://www.eje-online.org.ezproxy.library.wisc.edu/content/138/1/16
[17] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[18] Puel et al. 2011 Chronic Mucocutaneous Candidiasis in Humans with Inborn Errors of Interleukin-17 Immunity. Science. Vol 332. http://science.sciencemag.org/content/332/6025/65/tab-pdf
[19] National Organization for Rare Diseases (NORD). Hypoparathyroidism. https://rarediseases.org/rare-diseases/hypoparathyroidism/
[20] Mayo Clinic. Hypoparathyroidism. http://www.mayoclinic.org/diseases-conditions/hypoparathyroidism/basics/symptoms/con-20030780
[21] National Organization for Rare Diseases (NORD). Hypoparathyroidism. https://rarediseases.org/rare-diseases/hypoparathyroidism/
[22] Mayo Clinic. Addison's Disease. http://www.mayoclinic.org/diseases-conditions/addisons-disease/home/ovc-20155636
[23] NIH Institute of Diabetes and Digestive and Kidney Disease. Adrenal Insufficiency and Addison's Disease. https://www.niddk.nih.gov/health-information/health-topics/endocrine/adrenal-insufficiency-addisons-disease/Pages/fact-sheet.aspx
[24] NIH Institute of Diabetes and Digestive and Kidney Disease. Adrenal Insufficiency and Addison's Disease. https://www.niddk.nih.gov/health-information/health-topics/endocrine/adrenal-insufficiency-addisons-disease/Pages/fact-sheet.aspx
[25] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[26] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[27] Choudhary et al. 2012. Autoimmune Polyendocrinopathy- Candidiasis-Ectodermal Dystrophy. Journal of Clinical Aesthetic Dermatology. Vol 5.
[28] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[29] Choudhary et al. 2012. Autoimmune Polyendocrinopathy- Candidiasis-Ectodermal Dystrophy. Journal of Clinical Aesthetic Dermatology. Vol 5.
[30] Alessandra Fierabracci. 2016. Type 1 Diabetes in Autoimmune Polyendocrinopathy-Candidiasis-Ectodermal Dystrophy Syndrome (APECED): A “Rare” Manifestation in a “Rare” Disease. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4964482/
[31] Husebye et al. 2009. Clinical manifestations and management of patients with autoimmune polyendocrine syndrome type I. Journal of Internal Medicine. Vol 265. p. 514–529.
[32] Husebye et al. 2009. Clinical manifestations and management of patients with autoimmune polyendocrine syndrome type I.
Image References
[1] Life-Extending Hormone Protects Thymus Gland, Bolsters Body’s Immune Response. by NutritonReview.org. 2016. https://nutritionreview.org/2016/01/life-extending-hormone-protects-thymus-gland-bolster-bodys-immune-response/
[2] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome. New York Academy of Sciences. p 78.
[3] Figure 1. AIRE and autoimmunity from Immunology: Education and promiscuity. Nature. http://www.nature.com/nature/journal/v420/n6915/fig_tab/420468a_F1.html
[4] Kai Kisand & Pärt Peterson. 2015. Autoimmune Polyendocrinopathy Candidiasis Ectodermal Dystrophy. Journal of Clinical Immunology. Vol 35. p.
463–478.
[1] Finnish-German APECED Consortium. 1997. An autoimmune disease, APECED, caused by mutations in a novel gene featuring two PHD-type zinc-finger domains. Nature. https://www.ncbi.nlm.nih.gov/pubmed/9398840/
[2] Peterson et al. 2003. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy (APECED): a model disease to study molecular aspects of endocrine autoimmunity. Clinical Experimental Immunology.
[3] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome. Annals of the New York Academy of Science. http://onlinelibrary.wiley.com/doi/10.1111/j.1749-6632.2011.06308.x/epdf
[4] National Organization for Rare Disorders. Autoimmune Polyglandular Syndrome Type 1. https://rarediseases.org/rare-diseases/autoimmune-polyglandular-syndrome-type-1/
[5] Hayter and Cook. 2012. Updated assessment of the prevalence, spectrum and case definition of autoimmune disease. Autoimmunity Reviews. Vol 11. http://www.sciencedirect.com/science/article/pii/S1568997212000225
[6] National Institute of Allergy and Infectious Diseases. Autoimmune Polyglandular Syndrome Type 1 (APS-1). https://www.niaid.nih.gov/diseases-conditions/autoimmune-polyglandular-syndrome-type-1-aps-1
[7] Gardner et al. 2009. AIRE in the thymus and beyond. Current opinion in immunology. 21:582–589.
[8] Owen, Punt, Stranford, and Jones. 2013. Kuby Immunology 7th edition. p. 310
[9] Gardner et al. 2009. AIRE in the thymus and beyond. Current opinions in immunology.
[10] The Finnish-German APECED Consortium. 1997. An autoimmune disease, APECED, caused by mutations in a novel gene featuring two PDH-type zinc-finger domains. Nature genetics volume.
[11] Kisdand et al. 2010. Chronic mucocutaneous candidiasis in APECED or thymoma patients correlates with autoimmunity to Th17-associated cytokines. The Journal of Experimental Medicine.
[12] Laasko et al. 2010. Regulatory T cell defect in APECED patients is associated with loss of naive FOXP3+ precursors and impaired activated population. Journal of Autoimmunity.
[13] Sarkadi et al. 2014. Autoantibodies to IL-17A may be correlated with the severity of mucocutaneous candidiasis in APECED patients. Journal of Clinical Immunology.
[14]Seattle Children's Hospital. Autoimmune Polyendocrinopathy, Candidiasis, Ectodermal Dystrophy (APECED).http://www.seattlechildrens.org/healthcare-professionals/access-services/diagnostic-services/laboratories/immunology-diagnostic-laboratory/disorders/apeced/
[15] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[16] Betterle and Volpato. 1998. Adrenal and ovarian autoimmunity. European Journal of Endocrinology. Vol 138. http://www.eje-online.org.ezproxy.library.wisc.edu/content/138/1/16
[17] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[18] Puel et al. 2011 Chronic Mucocutaneous Candidiasis in Humans with Inborn Errors of Interleukin-17 Immunity. Science. Vol 332. http://science.sciencemag.org/content/332/6025/65/tab-pdf
[19] National Organization for Rare Diseases (NORD). Hypoparathyroidism. https://rarediseases.org/rare-diseases/hypoparathyroidism/
[20] Mayo Clinic. Hypoparathyroidism. http://www.mayoclinic.org/diseases-conditions/hypoparathyroidism/basics/symptoms/con-20030780
[21] National Organization for Rare Diseases (NORD). Hypoparathyroidism. https://rarediseases.org/rare-diseases/hypoparathyroidism/
[22] Mayo Clinic. Addison's Disease. http://www.mayoclinic.org/diseases-conditions/addisons-disease/home/ovc-20155636
[23] NIH Institute of Diabetes and Digestive and Kidney Disease. Adrenal Insufficiency and Addison's Disease. https://www.niddk.nih.gov/health-information/health-topics/endocrine/adrenal-insufficiency-addisons-disease/Pages/fact-sheet.aspx
[24] NIH Institute of Diabetes and Digestive and Kidney Disease. Adrenal Insufficiency and Addison's Disease. https://www.niddk.nih.gov/health-information/health-topics/endocrine/adrenal-insufficiency-addisons-disease/Pages/fact-sheet.aspx
[25] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[26] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[27] Choudhary et al. 2012. Autoimmune Polyendocrinopathy- Candidiasis-Ectodermal Dystrophy. Journal of Clinical Aesthetic Dermatology. Vol 5.
[28] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome.
[29] Choudhary et al. 2012. Autoimmune Polyendocrinopathy- Candidiasis-Ectodermal Dystrophy. Journal of Clinical Aesthetic Dermatology. Vol 5.
[30] Alessandra Fierabracci. 2016. Type 1 Diabetes in Autoimmune Polyendocrinopathy-Candidiasis-Ectodermal Dystrophy Syndrome (APECED): A “Rare” Manifestation in a “Rare” Disease. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4964482/
[31] Husebye et al. 2009. Clinical manifestations and management of patients with autoimmune polyendocrine syndrome type I. Journal of Internal Medicine. Vol 265. p. 514–529.
[32] Husebye et al. 2009. Clinical manifestations and management of patients with autoimmune polyendocrine syndrome type I.
Image References
[1] Life-Extending Hormone Protects Thymus Gland, Bolsters Body’s Immune Response. by NutritonReview.org. 2016. https://nutritionreview.org/2016/01/life-extending-hormone-protects-thymus-gland-bolster-bodys-immune-response/
[2] Kisand and Peterson. 2011. Autoimmune polyendocrinopathy candidiasis ectodermal dystrophy: known and novel aspects of the syndrome. New York Academy of Sciences. p 78.
[3] Figure 1. AIRE and autoimmunity from Immunology: Education and promiscuity. Nature. http://www.nature.com/nature/journal/v420/n6915/fig_tab/420468a_F1.html
[4] Kai Kisand & Pärt Peterson. 2015. Autoimmune Polyendocrinopathy Candidiasis Ectodermal Dystrophy. Journal of Clinical Immunology. Vol 35. p.
463–478.
This website was created by Julia Boles for Genetics 564, a genetics course at University of Wisconsin-Madison.
Contact: [email protected]
Last Updated: 5/1/2017
Contact: [email protected]
Last Updated: 5/1/2017


